If cannabis is so widely consumed among people suffering from depression, does that mean that marijuana and antidepressants go along together well? How do they actually interact?
How antidepressants work
Antidepressants are used for treating all types of depression, from mild to severe, but also for different mental disorders such as anxiety, ADHD, eating disorders, OCD and a few others. They can even be prescribed in combination with other medications.
There are several groups of antidepressants but in general, antidepressant therapy usually helps to regulate serotonin levels. Unfortunately, medication associated with serotonin regulation tends to cause restlessness, mania, emotional liability and sleeping problems in the long term.
These drugs are recommended by the doctors as the first choice for treating depression, along with cognitive therapy if necessary. However, the most popular antidepressants in the US and Canada such as Zoloft, Prozac and Lexapro tend to be overshadowed by a lot of controversies.
“Meanwhile, 30 years after Prozac was released, rates of depression are higher than ever.” – Olivia Goldhill, Quartz
A few meta-analyses and comprehensive review studies have found that these medications do not have (or have a very little) impact on mild and moderate short-term depression.
The big problem here is that antidepressants have a lot of adverse side-effects. Changes in weight, sleep, emotions, are just some of the reasons why patients stop using them.
Is this why people who suffer from depression tend to use cannabis more? What happens when we mix antidepressants with cannabis?
Research and anecdotal evidence on mixing weed with antidepressants
When it comes to mixing marijuana and antidepressants, we can conclude more from the testimonies of patients and their doctors than we can from the existing academic research and clinical trials. Sadly, academic and clinical databases have just a few reports on this topic.
Researchers from the Division of Child and Adolescent Psychiatry at the University of Connecticut Health Center made a review of published reports on cannabis and antidepressants interaction. As they pointed out, there have been only a few cases reported on adverse effects as a result of mixing cannabis and antidepressant drugs. (2)
There are several theories about why this might happen:
- There are no adverse effects
- They happen rarely or…
- They do happen but are not reported due to social stigma.
As of recently, there have been several reports on how CBD interacts with pharmaceuticals. These findings claim that CBD deactivates P450 liver enzymes, which metabolize the majority of the drugs we use today. (3)
Luckily for us, this interaction is noticeable only if we take higher doses of CBD, and it’s negligible in lower doses of 2-10 mg/day.
I’d also like to stress that some reports claim that older antidepressants tend to produce more adverse effects when combined with cannabis, however, newer generations of antidepressants reportedly have a lower risk of negatively interacting with cannabis.
Medical experts, speaking from their experience with patients using antidepressants in combination with cannabis, say that the biggest problem is the inability to know which adverse effects to expect from the combination.
But, what about patients themselves? I mean, anecdotal evidence has to account for something in cases where we lack scientific research.
To find out what patients who like to smoke cannabis while taking antidepressants have to say about their experience, I did a little research online and found some interesting threads.
A lot of patients say they usually don’t experience any adverse effects when combining SSRIs with marijuana.
For example, this thread was among the more interesting ones.
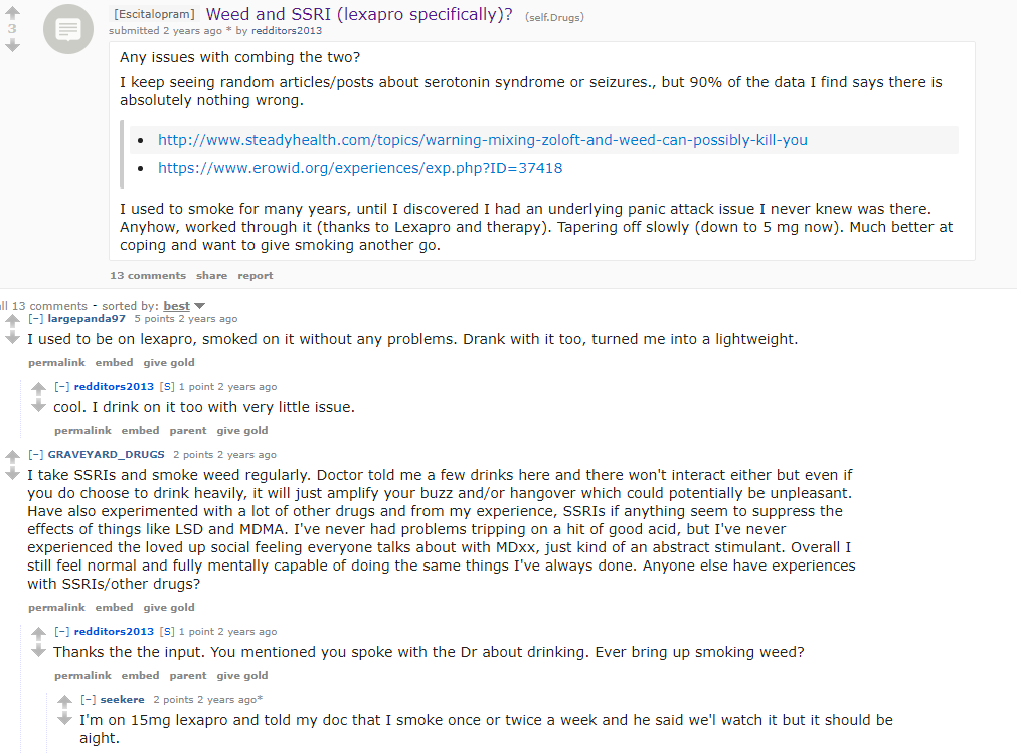
Here’s another user who had no issues:

As I previously mentioned in my article on marijuana and anxiety, both main cannabinoids found in cannabis (THC and CBD) can have very positive effects on anxiety and depression.
The downside is that cannabinoids produce biphasic effects. Too much THC can cause paranoia as well as increased anxiety. So, if you have previously experienced paranoia or a panic attack as a result of smoking weed or eating an edible, you should probably stay away from cannabis during your antidepressant therapy.
Since CBD reduces the psychoactive effects of THC, stick to CBD-rich strains or CBD oils. You can find a lot of CBD products on the market, but I advise you to get yours from a reputable dispensary and in the form of a whole plant extract.
More related posts
Marijuana and Depression: Can Weed Help You Make a Positive Change? — breaking down the studies on marijuana and depression and exploring the 10 best strains for managing symptoms of depression.
17 Truly High CBD Strains And Their Effects (The Complete List) — high CBD strains bring forth a heap of medical benefits and are awesome for treating depression. You should say “hi”.
How Does Cannabis Interact with Other Drugs — an overview of what happens if you mix weed with sedatives, antidepressants, antipsychotics, drugs for lowering blood pressure, and more.
References:
- Bricker JB, Russo J, Stein MB, Sherbourne C, Craske M, Schraufnagel TJ, Roy-Byrne P; Does occasional cannabis use impact anxiety and depression treatment outcomes?: results from a randomized effectiveness trial; Depression and Anxiety; August 2007; 24(6): 392-398
- Kaminer Y, Goldberg P, Connor DF; Psychotropic Medications and Substances of Abuse Interactions in Youth; Substance Abuse; July 2011; 31(1):53-57
- Bornheim LM, Everhart ET, Li J, Correia MA; Characterization of cannabidiol-mediated cytochrome P450 inactivation; Biochemical Pharmacology; March 1993; 45(6): 1323-1331







Tana March 28, 2018 at 4:17 am
I’ve experienced the panic attacks and paranoia While taking antidepressants and smoking weed. It scared the hell out of me and I would only take one or two small hits of Medical MJ to make sure I wouldn’t freak out! I quit taking the antidepressants and the MJ does just fine these days!
Gypsymoth November 29, 2018 at 5:43 am
I, and so have a few other people I have talked to, have had an interaction with marijuana and antidepressants; pyschotic episodes where complete loss with reality has happened, extreme agitation, anxiety, paranoia, and extreme insomnia. It has lasted a couple of days in a couple of the people. It seems to be a side effect of the vape type mm with the higher thc concentrations.
Smith April 26, 2019 at 6:43 pm
I am on prozac for 10 months now for anxiety. When I started taking prozac I didn't smoke weed much it was only once a week. But during the recent 3 months I was smoking almost daily.. that amplified my anxiety and sychphesical symptoms.. I am quitting weed for good, at least until I am done with the prozac ..
JJ November 21, 2019 at 7:48 pm
After smoking small amounts virtually every evening... for 15 years or so... I tried several SSRI drugs... for moderate anxiety and associated minor depression... they all gave me bad side effects... after stopping the SSRI's after only a week or so (2 tries recently)... I found that smoking my nightly bowl gave me an unpleasant feeling of anxiety and illness... Not sure if it was from an interaction... or if I finally just couldn't handle the weed anymore... will stop the smoking... and since CBD oil doesn't agree with me at all, nor do high CBD strains... that is not an option... I got some withdrawal effects when previously quitting the weed for only 3-4 days... tolerable but unpleasant... if anxiety comes back, I'll take some low dose Xanax or Ativan to get me over the hump... I have a healthy regard for the dangers of Benzo addiction...